Why (and how) we decided to submit a freedom of information request to NHS Trusts
In May this year I went along to observe a hearing at the Court of Protection. It’s something we at Compassion in Dying do sometimes as the decisions made by this court are relevant to the people we support.
The court deals with a wide range of matters, and most cases are not relevant to the work we do. But generally a case is relevant to our work if it’s about whether:
- the NHS should withdraw medical treatment, or
- a serious medical treatment decision is in a person’s best interests
Sometimes there are very specific cases about an advance decision to refuse treatment (ADRT) or lasting power of attorney (LPA) which may also be relevant.
I’ve recently been thinking about how we spend our time observing, analysing and using learnings from these cases… but that’s a separate blog post.
Why this hearing prompted an FOI request
The particular case I observed was about someone who’d made an ADRT, and specifically whether it was ‘valid’ and ‘applicable’ to their situation. The full judgment or a blog post about the case are worth reading if you have time as they set out the wider picture and context of the situation.
To summarise what was a complex case, there were some doubts about whether the person’s ADRT was valid and applicable to the situation they were in. The doubt came from multiple parties - but most relevant for us was that the NHS Trust who were caring for the person at the time questioned the ADRT. It transpired that there shouldn’t have been any doubt at all really but that even so, the matter should’ve been referred to the court much earlier than it was.
We know (from our helpline service) that people often have problems in hospitals when it comes to having ADRTs or LPAs accepted or followed by healthcare professionals. We have some idea of why this might happen but there is a knowledge gap in terms of knowing specifically what’s going wrong.
As the case was concluding, the NHS Trust implied their guidance on ‘Mental Capacity Act Advance Decisions and Advance Statements’ was at fault. They even submitted the particular policy and highlighted sections which they were going to update and improve as a result of the issues highlighted in the case:

This was the first Court of Protection case I’ve observed where an NHS Trust has admitted some key failings around their policies and procedures.
It made me wonder if these NHS TRUST policies could explain some of the poor practice we hear about.
Having had a chat with a colleague about the feasibility of submitting a freedom of information (FOI) request we decided as a team it was worth doing.
I think a key part of this decision was not committing up front to lots of follow-on work. We thought about it more as a ‘let’s try and see what we get’ idea.
How we submitted our FOI
I’m not a policy person, so had to lean on my policy expert colleagues on how to submit the FOI.
Given there are over 200 NHS Trusts (of varying descriptions) we decided to use WhatDoTheyKnow Pro to submit a batch FOI request.
This handy tool takes some load of the initial request work by submitting them all in a big batch to 135 NHS Foundation Trusts for example. It also manages the email back and forth with the NHS Trust information governance team which saves your email inbox from a bit of mess. So far, I think it’s a good tool and worth the £20/month cost.
Once we’d decided on the tool, we decided on submitting our FOI to the following NHS Trusts (or Health Boards):
- 14 NHS Scotland Healthboards
- 8 NHS Wales local Healthboards (includes 1 Trust)
- 135 NHS Foundation Trusts
- 57 NHS Hospital Trusts
We then decided on the FOI questions we’d ask. The below were what we thought would reveal the most useful information:
- Does the Trust have a policy which outlines responsibilities of healthcare professionals towards patients who have an advance decision to refuse treatment or lasting power of attorney?
- If there’s a dispute does the Trust have a process or course of action the person should follow?
- Does the Trust have someone responsible for overseeing compliance with the Mental Capacity Act?
What we’ve been sent (so far)
As it stands we’ve currently heard from:
- 85% NHS Foundation Trusts 🧐
- 85% NHS Hospital Trusts 🧐
- 100% NHS Scotland Healthboards ✅
- 100% NHS Wales local Healthboards ✅
Some responses are ‘long overdue’ which means the NHS Trust has breached the requirement to respond within 20 working days. We’ll try to chase but I think it’s possible we’ll just not hear back from some?
Having been sent a large number of policies from NHS Trusts - there are some early themes which are interesting and are already proving useful to the team.
I ran a half-day workshop with the team to go through these last week which I think was helpful to get everyone up to speed on what we’ve found so far.
Importantly I wanted to get a sense of the teams appetite and interest in what (if any) follow-up work we may want to do with what we’ve been sent.
Some early findings from 170ish NHS Trust policies
These findings are by no means final or complete as we’ve been sent at least 170ish PDF policy documents so far. Most of them are 15 - 20 pages long. As a result we’ve not done any sort of substantive analysis or documenting of what we’ve been sent.
Inconsistent policy naming
One of the quickest things I noticed was the inconsistencies with the names of policies we were being sent.
The most common type of policy was some form of policy for ‘complying with the Mental Capacity Act’. But even here there were differences - some for example included Deprivation of Liberty Safeguards (DOLS) and others had separate policies.
Some NHS Trusts had specific ADRT policies in addition to a broader Mental Capacity Act compliance policy. Where this was the case, we don’t have an answer as to why they have this… just that they do. For our purposes it’s probably the case that a Trust which has a dedicated policy on ADRTs is more likely to have good practice than one which doesn’t… but that could be a totally wrong hypothesis!
Different NHS staff policy authors
One very interesting finding is the differences between responsible NHS staff / authors of these policies.
It is not an unreasonable assumption to make sure an NHS Trust is following a specific law would suggest a specific named role would be needed to monitor compliance. And yet, look at this small selection of role titles of policy authors:
- Associate Director of Nursing for Safeguarding
- Head of Mental Health Law
- Associate Medical Director
- Safeguarding and Vulnerable Adult Lead Nurse
- Mental Health Act Manager
- Mental Capacity Act Lead
- Head of Legal Services
- Head of Safeguarding
- Clinical Lead End of Life Care
There is a quite a lot to unpick here, but it’s already useful in the sense that it gives our team a much more targeted way of escalating issues on behalf of our service users.
Interesting naming and policy history context
I found the below little snippet buried in the document version control section of a specific policy at Calderdale and Huddersfield NHS Foundation Trust.
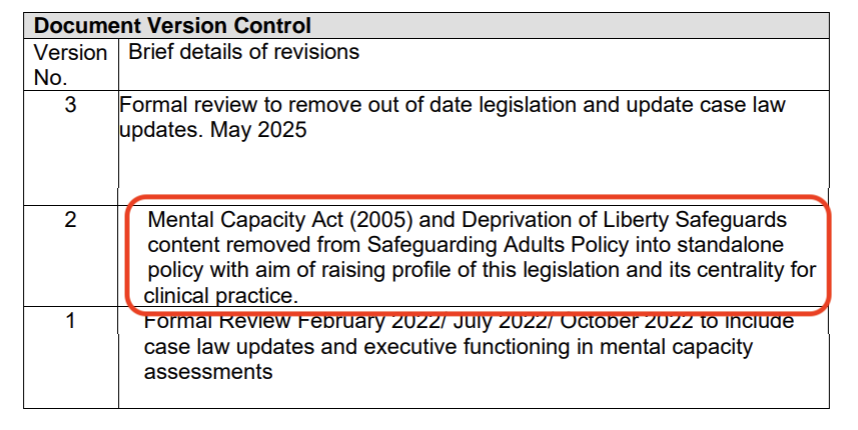
It suggests one reason why there may be a variation in policies and why many still sit under ‘safeguarding’ directorates within NHS Trusts.
Some NHS Trusts have detailed policies (with extras)
Just to drive home the above point about inconsistencies, whilst some NHS Trusts have pretty short and basic policies… there are some that appear to go above and beyond.
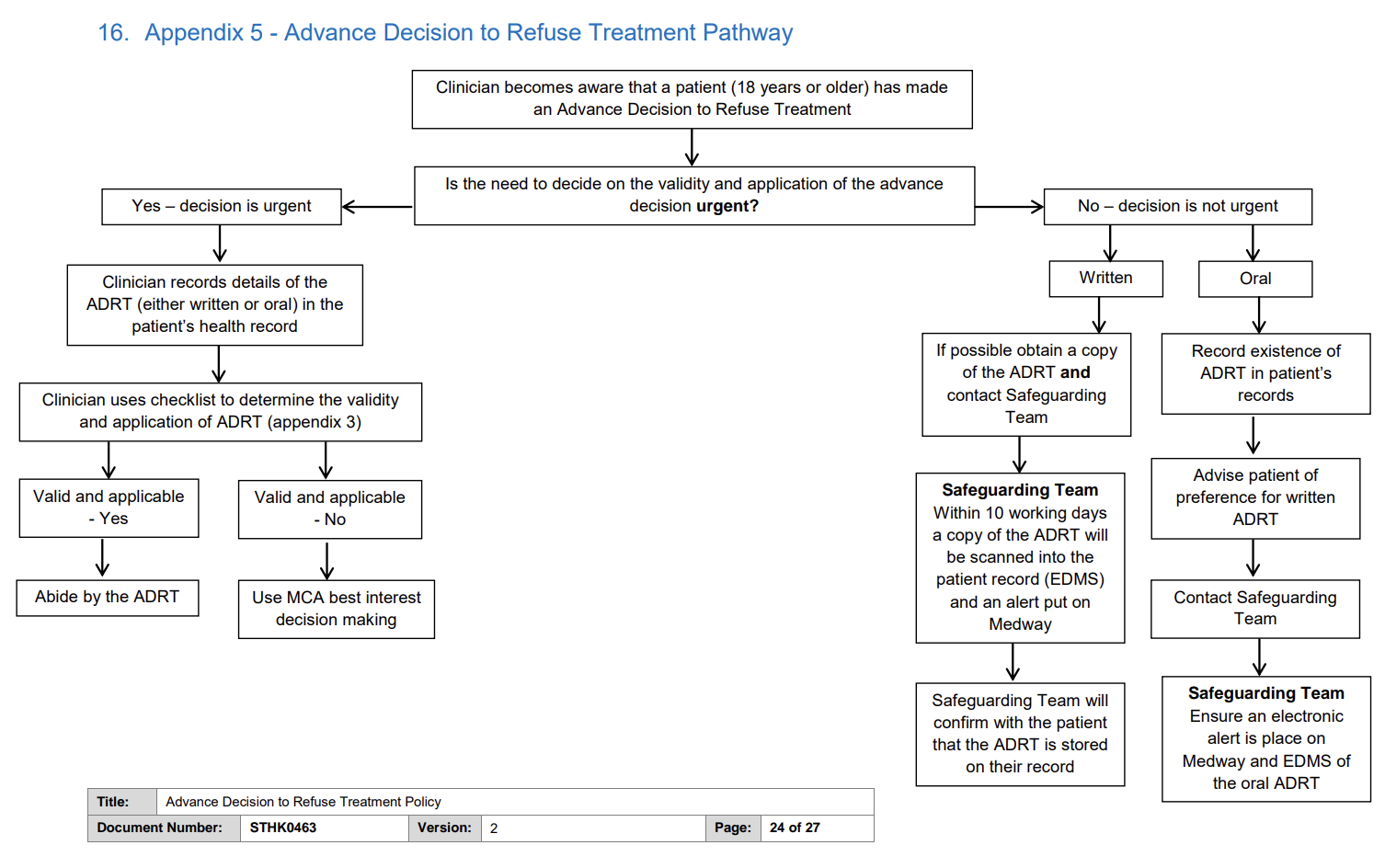
The above from Mersey and West Lancashire Teaching Hospitals NHS Trust is just one of several ‘extra’ documents within their policies which seem to suggest a thorough and rigorous approach to compliance with the Mental Capacity Act.
They (and some others) had things like:
- ADRT treatment pathways
- Capacity assessment forms and flowcharts
- Best interest meeting templates
- Template ADRT form
- ADRT flowcharts
- Advance Care Planning comparison tables
The dispute process was usually covered in some form
In response to our second FOI question, it did appear that policies addressed what to do where there was a disagreement between professionals themselves or with families.

What we plan to do now
In the workshop I mentioned we spent the biggest portion of the day discussing ideas of how we might use the results of our FOI.
Going back to the original idea, I stressed the importance of not committing up front to lots of follow-on work.
That being said, I wanted to give the team freedom to think up ideas about:
- What could be done
- How it might help the people we support
- How it might support our organisational policy goals
- How much work it might take for their ideas
It was a slightly rushed part of the day due to me being late for my own workshop… but here are the ideas we came up with as a team:
- Use the policies in our professional education and training work.
- Use the positive examples (of NHS Trust policies) to influence the ‘less good’ ones.
- Submit a similar FOI to primary care providers.
- Use this work as a showcase of our policy expertise - on social media, blog posts.
- Do some follow-up work with clinicians on behaviour change - and balance this with FOI results to see what most influences behaviours. Good policy ≠ Good practice.
- Contact (and help) the NHS Trusts with the worst policies to try and pre-empt problems for the people we support.
- Write a blog post about the work 😎.
- Conduct a full analysis of the policies and create some sort of ranking or coding of them to help staff use them.
- Create a searchable database of the policies for staff to use.
- Submit follow-up FOI to find out NHS Trust approaches to specific training on their policy.
- Pick 5 NHS Trusts to develop a relationship with and do follow-up work with because: Having policy AND relationship is probably better than JUST having the policy.
I like this list. There is a bit of crossover between a few of the ideas and we didn’t do as much exploration or fleshing out of details as I wanted. There also wasn’t much exploration of the work involved in each idea - maybe that was a bit ambitious, but I do think it’s a critical part of the next bit as we are a small team constantly struggling to deliver.
I prompted a bit of retrospective ‘dot voting’ a few days after the workshop and it looked like this idea was most popular:

I asked people to vote using different colour dots:
- Red dot - Impact for service users
- Blue dot - Impact on how people view us as an organisation
- Green dot - What excites you personally most
So, that’s where we are. From May - October this year. An idea formed, an FOI submitted and some early exploration of what’s next.
I like to think this isn’t where it stops, but even if so I’d consider it a good use of time. So long as we decide not to proceed actively and together (rather than start work and not finish).
The other good thing is that the results are already being used by the team to support people. Two cases so far:
- Sarah and Amber used the policy from Mid + South Essex Foundation Trust in some training they did with some of their staff.
- Sarah used the policy from a particular NHS Trust in an email to support someone’s request to have a medical device removed. The policy backed up that request.
Either way, hopefully this list grows!